Physiology Friday #311: Does Being Fitter Protect against Depression and Dementia?
What's good for the heart is good for the brain.
Greetings!
Welcome to the Physiology Friday newsletter.
Details about the sponsors of this newsletter and deals on products I love, including Ketone-IQ, Create creatine, Equip Foods, and ProBio Nutrition can be found at the end of the post.
The fitter you are, the less likely you are to die of nearly anything.
That’s not a controversial statement at this point.
The associations between cardiorespiratory fitness and a lower risk of cardiovascular disease, metabolic disease, cancer, and all-cause mortality are well established. I’ve written about that plenty before (you can find the latest example here).
But while the body-side benefits of fitness are widely appreciated, the brain side is still catching up in the broader conversation.
We already know that what is good for the heart is often good for the brain. Better vascular health, better metabolic health, better mitochondrial function, better inflammatory control… these are not body-only phenomena. The brain is downstream (technically upstream, directionally speaking) of all of them. So it’s not a stretch to think that better cardiorespiratory fitness may also confer some protection against mental disorders, neurodegeneration, or age-related cognitive decline.
That idea gets even more interesting when you make the important distinction that fitness is not the same thing as exercise. I say it’s interesting because there’s overwhelming evidence that participating in exercise and physical activity directly confers benefits to mental and cognitive health.
But exercise is the behavior. Fitness is, in part, the physiological result.
If higher cardiorespiratory fitness itself is associated with a lower risk of depression, dementia, or other neuropsychiatric conditions, that suggests something more than “people who exercise are healthier.” It suggests that the physiological machinery that allows someone to achieve and maintain better aerobic fitness (the integrated function of the heart, lungs, vasculature, skeletal muscle, and cellular energetics) may also track with better long-term brain and mental health.
The idea is compelling and logically sound, but as always, better to have data than assumptions.
A new systematic review and meta-analysis provides the most up-to-date evidence on the link between aerobic fitness and long-term brain health, asking whether people with higher cardiorespiratory fitness are less likely to go on to develop mental disorders or dementia later in life.1
This was a meta-analysis of 22 cohort studies involving more than 4 million participants, generally between 18 and 64 years old, who had fitness assessed at baseline and were then followed for anywhere from 4 to 29 years. Fitness was measured in several different ways across studies. Some cohorts used direct VO2 max testing, others used indirect maximal or submaximal exercise tests, and others used estimated or field-based metrics like METs, peak workload, exercise duration, or distance covered. So while the paper is about cardiorespiratory fitness, it is not exclusively about directly measured VO2 max (this has become an especially important nuance to point out, since some folks on social media get angry if one doesn’t specify).
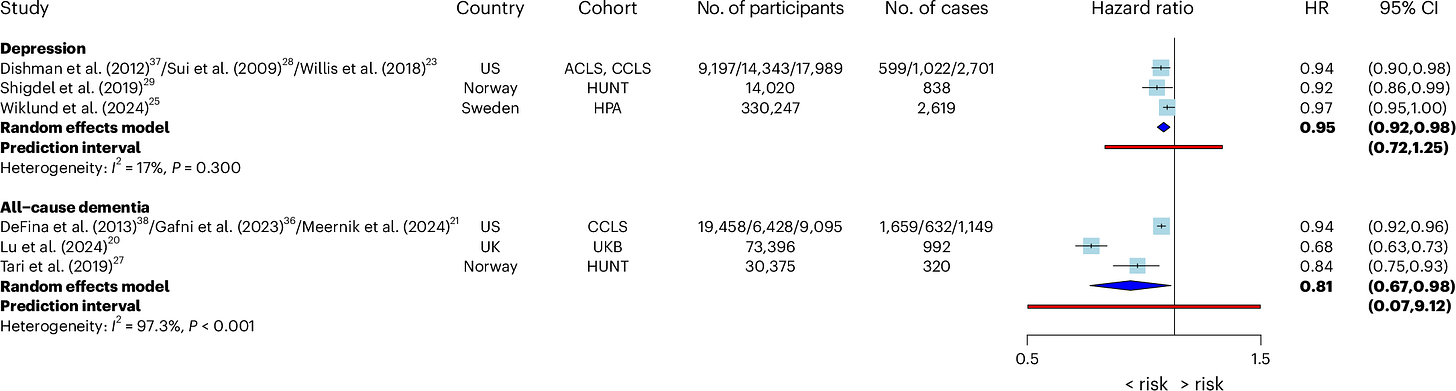
Across studies, higher cardiorespiratory fitness was associated with a substantially lower future risk of depression, all-cause dementia, and psychotic disorders, but not clearly with anxiety.
Compared to people with low fitness, those with high fitness had:
a 36% lower risk of depression.
a 39% lower risk of all-cause dementia.
a 29% lower risk of psychotic disorders.
And when fitness was analyzed continuously rather than categorically, each 1-MET (3.5 ml/kg/min) increase in cardiorespiratory fitness was associated with a 5% lower risk of depression and a 19% lower risk of dementia. This is perhaps the more important stat in my opinion, because it shows how a small but meaningful fitness bump affects long-term disease risk (we don’t have hard numbers for the low- versus high-fitness categories, unfortunately).
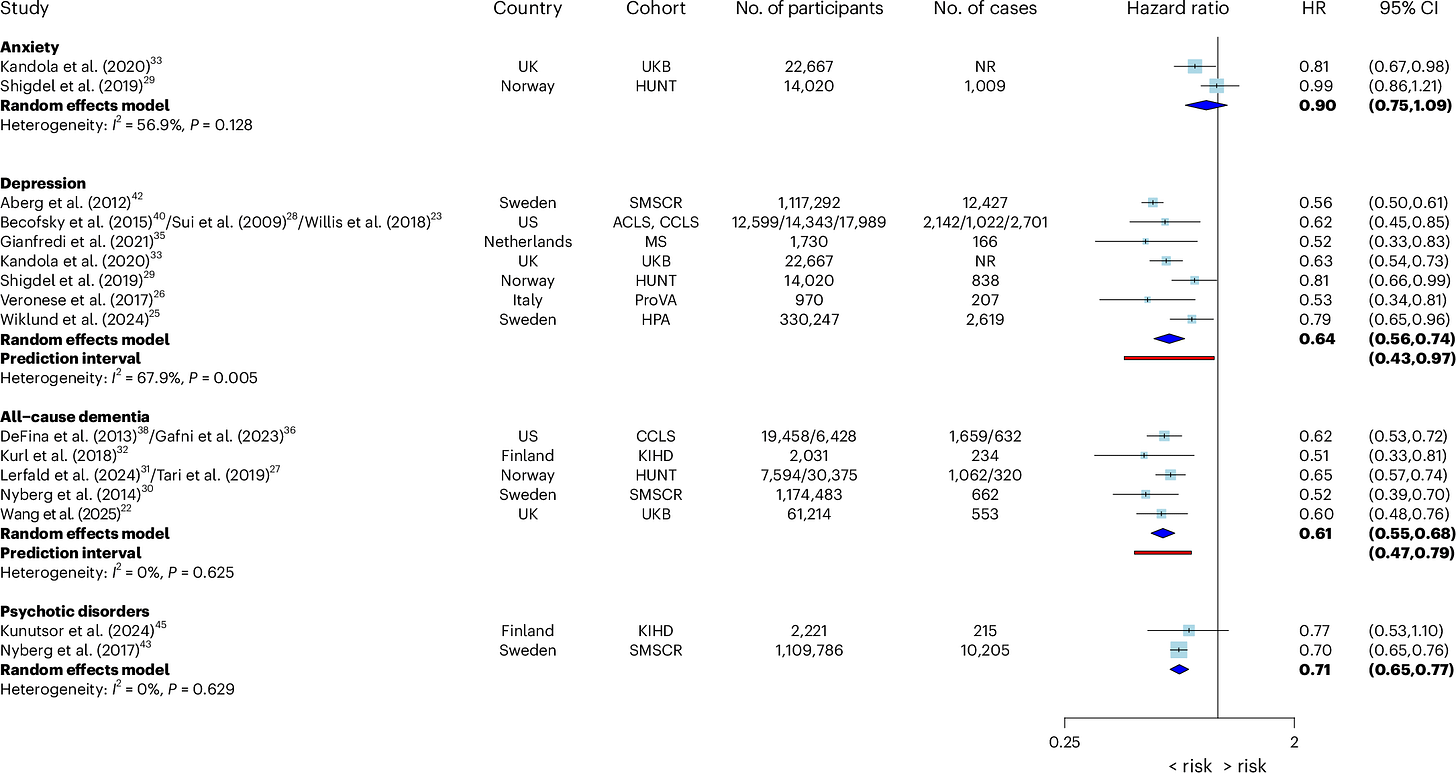

The results were also broadly similar across several subgroup analyses, including people above and below age 50, men and women, and studies using indirect maximal or submaximal testing rather than direct lab-based VO2 max measures.
The authors also discussed several outcomes that were not meta-analyzed because only one or two studies were available. Even so, those individual studies suggested that higher fitness may also be associated with lower risk of bipolar-related disorders, dissociative disorders, obsessive-compulsive and stressor-related disorders, somatic symptom disorders, sleep apnea, as well as anxiety and ADHD in children. Depression in girls also appeared lower with higher fitness.
So taken at face value, the signal is broad: higher cardiorespiratory fitness seems to track with lower risk across a wide range of psychiatric and neurocognitive outcomes.
That said, this is still observational evidence, and observational evidence always comes with some limitations.
The first is what’s known as residual confounding. Even in well-adjusted cohort studies, there are always variables that are incompletely captured or not captured at all.
Factors like genetic predisposition, chronic pain, other comorbidities, social support, smoking, diet, and general physical activity habits are potential confounders. It is entirely possible that higher-fitness individuals differ from lower-fitness individuals in multiple ways beyond fitness itself, and some of those differences could independently influence mental health or dementia risk.
The second is reverse causation, which is especially important here.
Early or subclinical symptoms of depression, neurodegeneration, or other psychiatric disease may reduce motivation, physical activity, energy levels, or exercise capacity before a formal diagnosis is ever made. In that scenario, lower fitness would not necessarily cause later disease. It might instead be an early marker of disease already beginning to develop.
The included studies tried to address this by excluding people with diagnosed conditions at baseline, but that only goes so far. Disease can exist for years before diagnosis, especially in dementia.
So while the associations are compelling, they are not proof that improving fitness will directly prevent depression, dementia, or psychotic disorders. To know that, we’d need study designs that measure aerobic fitness at several time points over years to decades to see whether increasing or decreasing fitness is associated with a lower or higher disease prevalence. Ideally, we’d want a randomized controlled trial lasting two decades or more… a guy can dream.
And to the authors’ credit, they do not overclaim. They conclude that higher cardiorespiratory fitness appears to be associated with a lower risk of several mental and neurocognitive disorders, and cardiorespiratory fitness may be a useful candidate marker for risk stratification.
The biological plausibility is real
Even though causality is not established in an observational study like this, the biology here is not hand-wavy. There are several plausible mechanisms linking higher cardiorespiratory fitness to better mental and neurocognitive outcomes, including greater neuroplasticity (the brain’s ability to “rewire” itself), improved brain blood flow and vascular function, reduced inflammation and oxidative stress, and a more stable response to stress. There’s also broader exercise-related pathways involving brain-derived neurotrophic factor (BDNF) signaling (Dr. Rhonda Patrick is the go-to source here), angiogenesis, mitochondrial health, immune regulation, and psychosocial factors like self-efficacy and social support. It’s impossible to say “this one mechanism explains the benefit,” as it’s likely a combination of several factors that explain why fitness (and exercise) have tight links to brain health.
To me, one of the most compelling pieces of the story is the structural brain literature.
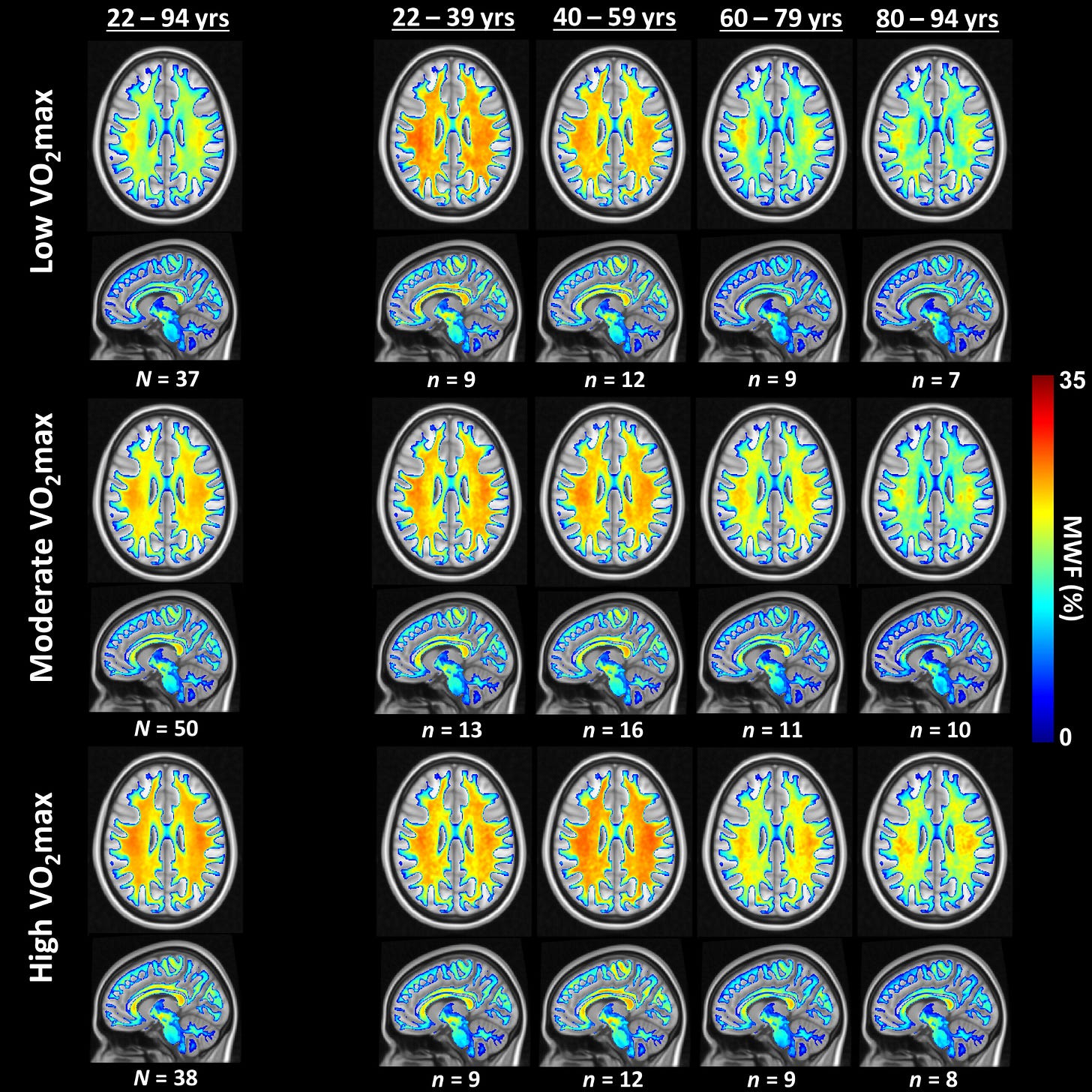
In an earlier newsletter, I covered a study suggesting that the relationship between aerobic fitness and brain health may be partly structural, not just functional. That study directly measured both VO2 max and brain myelin content (myelin being the protective and super-important insulation around our neurons) in 125 cognitively normal adults across two aging cohorts. Higher aerobic fitness was associated with greater myelination across much of the brain, with the strongest differences showing up in middle-aged and older adults. Furthermore, fitter people appeared to reach peak myelination later and then lose it more slowly with age. Across the full sample, myelin peaked around age 31, but in the lowest-fitness group, it peaked before age 22, whereas in the highest-fitness group, it didn’t peak until around age 41. Higher cardiorespiratory fitness has also been associated with less grey and white matter deterioration in adults across the lifespan.
Again, this is not proof that raising fitness prevents dementia. But it strengthens the idea that cardiorespiratory fitness may be a meaningful marker of long-term brain-aging risk.
Mental disorders and neurodegeneration are complex, multifactorial, and deeply heterogeneous. So I am not going to be the person who says, “exercise is the answer.”
Maybe it is one answer. And maybe it is an important one. But I am generally skeptical of the overly simplistic line that “exercise is just as good as medication for depression” (or insert your favorite mental health condition). Improving mood, reducing depressive symptoms, and treating major clinical depression are not interchangeable ideas. And while there is good evidence that exercise and physical activity can help with depressive symptoms, I think the health and fitness world sometimes overshoots by making it sound as though all it takes is a little movement. That is too reductive for a condition as complex as depression.
With dementia and Alzheimer’s disease, I am somewhat more bullish on the role of activity and fitness. Not because I think they are magic bullets, but because the pathways involved, including vascular dysfunction, metabolic dysfunction, inflammation, neurodegeneration, and reduced cerebral blood flow, are exactly the kinds of processes that fitness influences. If there is one lifestyle-related trait I would want on my side for healthy brain aging, high cardiorespiratory fitness would be near the top of the list.
And despite VO2 max and cardiorespiratory fitness getting some pushback lately as “not true longevity markers,” I still do not see the case against them.
If anything, the opposite seems to be happening. The evidence continues to accumulate that cardiorespiratory fitness is associated not only with lower risk of physical disease and premature death, but also with better brain health, lower dementia risk, and perhaps lower risk of certain mental disorders as well.
And that matters because healthspan is not only about how well the body can hold up with age, but also about the brain that comes along for the ride (and is really in the driver’s seat).
Thanks for reading. See you next Friday.
~Brady~
Ketone-IQ is high-performance energy in a bottle. I use it for post-exercise recovery along with enhancing focus, mood, and cognition. Take 30% off your order.
Create is the first “modern creatine” brand. They sell a wide range of creatine monohydrate gummies—and yeah, their gummies actually contain creatine, unlike some other brands. They’re giving my audience 20% off their order.
ProBio Nutrition—the all-in-one supplement that I use every single day—is offering 20% off. My preference is the tangy orange flavor, but they also sell an unflavored “smoothie booster” that’s great in a shake, smoothie, or juice.
Equip Foods makes some of the cleanest, best-tasting protein products around. I am absolutely obsessed with their Prime grass-fed protein bars (the peanut butter ones are to die for). Take 35% off a subscription.






I definitely feel better for exercising. When I get to the top of a hill the blood pumping, breathing heavy I am feeling pumped. Also lifting heavy weights. Currently listening to Dr Tommy Woods whom I will buy his book The Stimulated Mind. The brain's white matter stimulated by RT and grey matter aerobic. Mother-in-Law 90yo now sliding fast with dementia & maybe depression is hard to swallow and that is one reason why fitness people are trying to save themselves from a suffering ending. Only bc I am now 58yo I am aware of this vs early decades exercising was just plain fun, exciting and exhilarating.